What Is a Computed Tomography (CT) Scan?
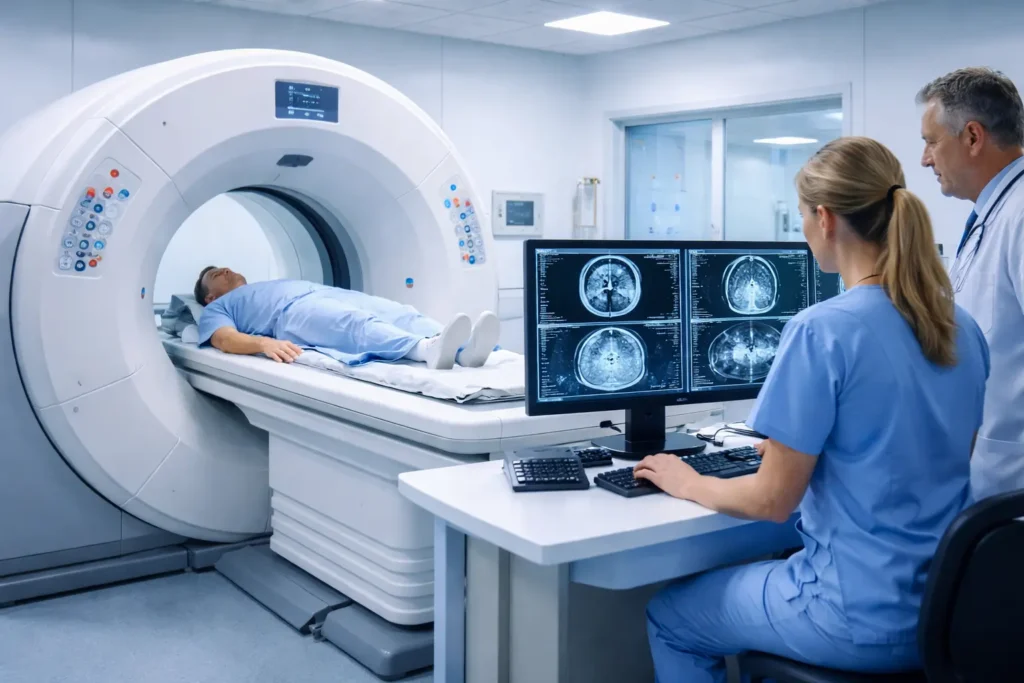
A Computed Tomography (CT) scan — also called a CAT scan (Computerized Axial Tomography) — is a sophisticated diagnostic imaging test that uses a series of X-ray measurements taken from different angles around your body to produce detailed cross-sectional images (slices). These slices can be digitally combined by a computer to generate three-dimensional images of your bones, soft tissues, blood vessels, and organs.
Unlike a conventional X-ray, which produces a single flat image, a Computed Tomography scan captures dozens to hundreds of individual slices. This allows radiologists to see inside your body with far greater clarity, identifying abnormalities that would be invisible or ambiguous on a standard X-ray.
CT scans are among the most widely used imaging tools in modern medicine. In the United States alone, more than 85 million CT examinations are performed annually.
A Brief History: From Nobel Prize to Modern Scanner
The CT scanner was invented independently by British engineer Godfrey Hounsfield and South African physicist Allan Cormack, who jointly received the Nobel Prize in Physiology or Medicine in 1979. The first clinical CT scanner — known as the EMI scanner — was installed at Atkinson Morley Hospital in London in 1971. That first machine took approximately 9 days per slice to reconstruct an image. Today’s photon-counting CT scanners complete a full body study in under 30 seconds.
How CT Works: The Physics Simplified
Here is a step-by-step breakdown of what happens inside the CT machine:
- You lie on a motorized scanning table that slides through a large ring-shaped device called the gantry.
- Inside the gantry, an X-ray tube rotates 360 degrees around your body, emitting a fan-shaped beam of ionizing radiation.
- A detector array on the opposite side of the gantry captures the X-ray beams after they pass through your body. Different tissues absorb X-rays at different rates — dense bone absorbs more, soft tissue less, air almost none.
- A powerful computer workstation processes these thousands of detector readings using a mathematical technique called tomographic reconstruction to build a cross-sectional image.
- Each image is measured in Hounsfield Units (HU): bone is approximately +400 HU, water is 0 HU, fat is approximately -100 HU, and air is -1,000 HU. These values determine the grayscale appearance of the final image.
- A radiologist (or radiographer/CT technologist) reviews the images, typically on a DICOM workstation, and writes a formal report.
CT vs. Other Imaging Modalities: The Comparison Table
One of the most common questions patients ask is: ‘Why a CT scan and not an MRI or ultrasound?’ The table below provides a direct comparison:
| Feature | CT Scan | MRI | Ultrasound | X-Ray |
| Radiation | Yes (low-dose ionizing) | No | No | Yes (very low) |
| Best For | Bone, chest, emergency | Soft tissue, brain, spine | Organs, blood flow | Bone fractures, lungs |
| Scan Speed | 5-10 minutes | 30-60 minutes | 10-30 minutes | 5-10 minutes |
| Claustrophobia Risk | Low (open doughnut) | High (enclosed tunnel) | None | None |
| Average Cost (US) | $300-$6,000 | $400-$12,000 | $100-$1,000 | $50-$400 |
| Soft Tissue Detail | Good | Excellent | Moderate | Poor |
| Contrast Needed | Sometimes (iodinated) | Sometimes (gadolinium) | Rarely | No |
Key takeaway: CT excels at speed, bone detail, and emergency imaging. MRI offers superior soft tissue contrast without radiation. Ultrasound is ideal for real-time imaging and is safe in pregnancy. X-ray is best for quick, simple bone assessments.
Why Would You Need a Computed Tomography Scan? (Clinical Applications)
Your doctor may order a CT scan for a wide variety of reasons. Below are the most common clinical uses, organized by urgency and body system.
Diagnosing Emergencies (Trauma, Stroke, Internal Bleeding)
CT is the workhorse of emergency radiology. Its speed — a full body trauma scan in under 60 seconds — makes it indispensable in life-threatening situations. Common emergency indications include:
- Stroke: CT rapidly distinguishes ischemic stroke (blocked artery) from hemorrhagic stroke (bleeding), which determines whether a clot-busting drug (tPA) can be safely administered.
- Head trauma: Identifies skull fractures, epidural/subdural hematomas, and brain contusions following accidents or falls.
- Internal bleeding: Detects hemorrhage in the chest, abdomen, or pelvis after blunt trauma.
- Pulmonary embolism (PE): CT pulmonary angiography (CTPA) is the gold standard for diagnosing blood clots in the lungs — a potentially fatal emergency.
- Aortic dissection: A tearing of the aorta’s inner wall, identifiable within minutes on CT angiography (CTA).
Cancer Detection, Staging & Treatment Monitoring
CT is fundamental to oncology at every stage of the cancer journey:
- Detection: Identifying lung nodules, liver masses, lymph node enlargement, and adrenal lesions.
- Staging: Determining whether cancer has spread (metastasized) to lymph nodes or distant organs — essential for treatment planning.
- Treatment response: Comparing tumor size before and after chemotherapy or radiation therapy.
- Surveillance: Monitoring for cancer recurrence after treatment.
- Biopsy guidance: CT-guided needle biopsy allows sampling of deep-seated tumors without open surgery.
Imaging Specific Body Parts
Head & Brain
CT of the head can detect: stroke and hemorrhage, brain tumors (primary and metastatic), hydrocephalus (fluid buildup), head trauma and skull fractures, sinusitis and sinus disease, and thyroid nodules.
Chest & Heart
Chest CT provides detailed evaluation of: lung nodules and masses, pulmonary embolism (using CT pulmonary angiography), pneumonia and lung infections, emphysema and interstitial lung disease, coronary artery calcium score (risk of heart disease), and cardiac CT for coronary artery stenosis.
Low-dose CT (LDCT) lung cancer screening is now recommended annually for high-risk adults aged 50-80 with a 20 pack-year smoking history.
Abdomen & Pelvis
Abdominal/pelvic CT is one of the most commonly ordered scans, used for: kidney stones (renal calculi), appendicitis, diverticulitis, Crohn’s disease and colitis, liver masses and gallbladder disease, pancreatitis, and CT colonography (virtual colonoscopy) for polyp detection.
Bones & Spine
CT surpasses plain X-ray for complex fractures, joint erosions in rheumatoid arthritis, bone tumors, spinal disc disease and nerve compression, and gout (showing uric acid crystal deposits).
Vascular Imaging
CT Angiography (CTA) maps blood vessels to diagnose: abdominal aortic aneurysm (AAA), carotid artery stenosis, peripheral arterial disease, and deep vein thrombosis (DVT).
Types of CT Scanners & Technologies
Helical (Spiral) CT — The Modern Standard
Modern CT scanners use helical (or spiral) technology, in which the table moves continuously while the X-ray tube rotates simultaneously. This creates a continuous spiral dataset of the entire body region, dramatically reducing scan time compared to older step-and-shoot (sequential) CT, where the table moved incrementally between each rotation. Helical CT is the technology behind virtually every CT scanner in use today.
Multi-Detector CT (MDCT)
Current scanners use multiple detector rows (from 16 to 320+ rows) to acquire many slices per gantry rotation. A 320-detector scanner can image the entire heart in a single beat. Key parameters include:
- Slice thickness: Thinner slices (down to 0.5 mm) provide higher resolution for small structures.
- Pitch: The ratio of table movement to beam width — higher pitch = faster scan but lower dose.
- kVp (tube voltage): Typically 80-140 kV; lower kVp reduces dose but may reduce image quality.
- Tube current (mA): Higher mA = less image noise but more radiation.
Advanced CT Techniques
- Dual Energy CT (Spectral CT): Uses two X-ray energy levels simultaneously to better characterize materials — distinguishing uric acid kidney stones from calcium stones, or iodine from hemorrhage. Also known as Spectral CT.
- CT Perfusion: Measures blood flow through the brain (in stroke) or heart muscle (in coronary artery disease) by tracking how contrast moves through tissue over time.
- High-Resolution CT (HRCT): Uses very thin slices and specialized reconstruction for detailed evaluation of lung diseases such as pulmonary fibrosis and bronchiectasis.
- PET-CT: Combines a CT scan with a Positron Emission Tomography scan. The PET component shows metabolic activity (e.g., highly active cancer cells), while CT provides precise anatomical localization. Widely used in cancer staging.
- CT Angiography (CTA): Uses IV contrast timed to arterial or venous filling to create detailed 3D maps of blood vessels.
Future Innovations: Photon-Counting CT & AI Reconstruction
The next frontier in CT technology is already arriving in leading medical centers:
- Photon-Counting CT (PCD-CT): Unlike conventional detectors that measure total X-ray energy, photon-counting detectors measure the energy of individual X-ray photons. This enables higher spatial resolution (sharper images), lower radiation dose, reduced image noise, and better material characterization — all simultaneously. The FDA cleared the first photon-counting CT system in 2021, and clinical adoption is rapidly expanding.
- AI-Based Image Reconstruction: Deep learning algorithms (such as Canon’s AiCE and Siemens’ Deep Resolve) can reconstruct high-quality diagnostic images from lower-dose scans, potentially reducing radiation exposure by 50-80% compared to traditional filtered back-projection reconstruction.
- Spectral Photon-Counting CT: Combines the advantages of dual-energy CT and photon-counting detectors, enabling unprecedented tissue characterization without additional radiation.
Contrast Media: Dyes That Make the Invisible Visible
Many CT scans use a contrast agent (commonly called ‘contrast dye’ or ‘contrast medium’) to enhance the visibility of blood vessels, organs, and abnormal tissues. Contrast works by temporarily altering the X-ray absorption of the target tissue, making it appear brighter (hyperdense) on the image.
Types of Contrast Media
- Intravenous (IV) iodinated contrast: The most common type. Injected via an IV catheter into a vein (usually the arm), it circulates through the bloodstream and enhances vascular structures and organs. Used for CT angiography, abdominal CT, chest CT, and brain CT.
- Oral contrast: Dilute iodinated or barium sulfate solution swallowed by the patient before the scan to outline the gastrointestinal tract. Useful for abdominal/pelvic CT to distinguish bowel from other structures.
- Rectal contrast: Administered via enema to opacify the colon and rectum. Used for pelvic CT and CT colonography.
- Bolus injection: IV contrast is typically injected rapidly (bolus) using an automated power injector at a rate of 2-5 mL/second to ensure peak arterial or venous enhancement.
Side Effects & Allergic Reactions
Most patients tolerate IV contrast without any adverse effects. However, reactions can occur and range from mild to life-threatening. Your radiology team is trained to manage all types of reactions.
| Severity | Symptoms & Signs |
| Mild (most common) | Metallic taste, warmth/flushing, nausea, itching, hives (urticaria), sneezing |
| Moderate | Severe vomiting, marked hives, bronchospasm (wheezing), facial edema, hypotension |
| Severe / Anaphylaxis (rare) | Life-threatening: laryngeal edema, severe bronchospasm, cardiovascular collapse, loss of consciousness. Rate: ~1 in 170,000 |
| Delayed Reaction | Skin rash, fatigue, or nausea appearing 1 hour to 1 week after contrast injection |
If you have had a previous allergic reaction to iodinated contrast, inform your doctor. Pre-medication with corticosteroids (e.g., prednisone) and antihistamines (e.g., diphenhydramine) can significantly reduce the risk of a repeat reaction.
Kidney Function & Contrast-Induced Nephropathy (CIN)
Iodinated contrast media are primarily excreted by the kidneys. In patients with pre-existing kidney disease (reduced GFR), contrast can occasionally worsen kidney function — a condition formerly called contrast-induced nephropathy (CIN), now more accurately termed contrast-associated acute kidney injury (CA-AKI).
Key points on CIN:
- Risk is primarily significant in patients with severe chronic kidney disease (eGFR < 30 mL/min/1.73m2).
- Risk is greatly reduced by adequate pre-hydration (IV saline before and after the scan).
- Metformin (a common diabetes medication) should be withheld for 48 hours after contrast in patients with kidney disease, as contrast can cause lactic acidosis in rare cases.
- The risk of CIN is often overstated; major radiology societies (ACR, European Society of Urogenital Radiology) have revised guidelines to reflect that the risk in patients with mildly reduced kidney function is lower than previously thought.
Always inform your doctor if you have diabetes, kidney disease, or are taking Metformin before any contrast CT scan.
Understanding Radiation Risks
Radiation safety is one of the most important — and most misunderstood — aspects of CT scanning. CT uses ionizing radiation, meaning X-rays have enough energy to ionize atoms in tissues, which can potentially cause DNA damage. Understanding the actual magnitude of this risk is essential for informed decision-making.
How Much Radiation Does a CT Scan Deliver?
Radiation dose is measured in millisieverts (mSv) — a unit that accounts for the type of radiation and its biological effect. We are all exposed to natural background radiation (from cosmic rays, radon gas, and food) continuously. The table below puts CT doses in context:
| Procedure / Source | Effective Dose (mSv) | Equivalent Background Radiation |
| Chest X-ray | 0.1 mSv | ~10 days |
| Mammogram | 0.4 mSv | ~7 weeks |
| Head CT | 2 mSv | ~8 months |
| Chest CT (standard) | 7 mSv | ~2 years |
| Chest CT (low-dose LDCT) | 1.5 mSv | ~6 months |
| Abdomen & Pelvis CT | 10 mSv | ~3 years |
| Coronary CT Angiography | 6-12 mSv | ~2-4 years |
| Annual Background (US avg.) | 3 mSv | Baseline |
| Cross-country flight (roundtrip) | 0.03 mSv | ~3 days |
The ALARA principle (As Low As Reasonably Achievable) guides radiology practice. Modern CT protocols are continually optimized to deliver the minimum dose needed for a diagnostic-quality image.
Long-Term Cancer Risk: Putting It in Perspective
The theoretical long-term cancer risk from CT radiation is based on the linear no-threshold (LNT) model, which extrapolates from high-dose radiation exposures (e.g., atomic bomb survivors) to the low doses used in CT. However, this model is disputed for very low doses, and many radiation biologists argue that the actual risk at CT doses may be lower than the model predicts.
Practical estimates based on the LNT model:
- A single abdominal/pelvic CT (10 mSv) is associated with an estimated lifetime attributable risk (LAR) of cancer of approximately 1 in 2,000 — compared to the baseline cancer risk in the general population of roughly 1 in 3.
- For most patients undergoing a clinically indicated CT scan, the benefit of accurate diagnosis far outweighs this small theoretical risk.
- Repeated CT scanning (e.g., in patients with Crohn’s disease or cancer surveillance) should prompt discussion with your doctor about whether alternative imaging (MRI, ultrasound) could reduce cumulative dose.
Special Populations: Children & Pregnant Patients
Pediatric CT — The ‘Image Gently’ Campaign
Children are more radiosensitive than adults because their cells are dividing more rapidly, and they have a longer lifetime ahead for any radiation-induced cancer to develop. The Image Gently campaign, launched by the Society for Pediatric Radiology and endorsed by the American College of Radiology (ACR), advocates for:
- Reduction of CT dose parameters (kVp, mA) in pediatric patients.
- Elimination of unnecessary repeat imaging.
- Substituting MRI or ultrasound where clinically equivalent.
- Scanning only the indicated region (avoiding ‘routine’ full-body scans in children).
CT During Pregnancy
CT during pregnancy requires careful risk-benefit assessment. Key facts:
- Fetal radiation risk from head or chest CT is negligible, as the uterus is outside the primary beam and absorbed dose to the fetus is very low (<0.1 mSv).
- Abdominal/pelvic CT delivers a higher fetal dose (1-50 mSv, depending on technique), which may be acceptable in genuine emergencies (e.g., suspected appendicitis, pulmonary embolism, trauma).
- MRI (without gadolinium contrast) is generally preferred over CT for non-urgent abdominal imaging in pregnancy.
- Iodinated IV contrast should be avoided in pregnancy unless essential, as there is theoretical concern about fetal thyroid suppression.
- Always inform the CT technologist and your doctor if you are pregnant or think you may be pregnant.
Preparing for Your CT Scan
Proper preparation ensures image quality, reduces the risk of complications, and makes your experience more comfortable. Follow your radiology department’s specific instructions, as they may vary by scan type.
Food, Drink & Medications
- Non-contrast CT: Usually no preparation needed. You can eat and drink normally.
- CT with IV contrast (fasting): You should generally not eat solid food for 3-4 hours before the scan. You may drink clear liquids (water, clear juice) up to 1-2 hours before.
- CT with oral contrast: You may be asked to drink contrast preparation (a diluted barium or iodine solution) 1-2 hours before the scan. Follow your department’s specific instructions.
- CT colonography: Requires a full bowel preparation (laxative cleanse) the evening before, similar to colonoscopy preparation.
- Metformin: If you take Metformin for diabetes and will be receiving IV contrast, your doctor may instruct you to withhold it for 48 hours after the scan.
- Blood thinners: No change is needed unless a biopsy is planned as part of the procedure.
Clothing & Metal Objects
You will likely be asked to change into a hospital gown. You must remove all metal objects before entering the CT scanner, including:
- Jewelry: Rings, necklaces, earrings, bracelets, and body piercings.
- Dentures and removable dental work (for head/neck scans).
- Eyeglasses.
- Hearing aids.
- Metal zips, belts, and underwire bras (if scanning the chest or abdomen).
What to Tell Your Doctor Before Your Scan
Always disclose the following to your referring doctor and the radiology team:
- Pregnancy or possible pregnancy.
- Previous allergic reactions to contrast dye, iodine, or shellfish (note: shellfish allergy is not a reliable predictor of contrast allergy, but should still be mentioned).
- Kidney disease or reduced kidney function (bring recent blood test results showing your eGFR/creatinine if possible).
- Diabetes — especially if taking Metformin.
- Asthma or other respiratory conditions (increases risk of contrast reactions slightly).
- All current medications, particularly Metformin, NSAIDs, and nephrotoxic drugs.
- Claustrophobia or significant anxiety (you may be offered a mild oral sedative).
- Presence of metallic implants: Note that unlike MRI, most metallic implants (pacemakers, joint replacements, surgical clips) are safe in CT. However, they can cause streak artifacts (see Section 8). Inform the team regardless.
What to Expect During the CT Scan Procedure
Step-by-Step: From Check-In to Discharge
- Arrival & registration: Check in at the radiology department. Complete consent forms and a medical history questionnaire.
- Preparation: Change into a gown, remove metal objects, and store valuables. If contrast is planned, a nurse or technologist will insert an IV catheter (usually in the antecubital fossa — the inside of your elbow).
- Pre-scan oral contrast: If required, you will drink the contrast solution now and wait 45-60 minutes for it to reach your bowel.
- Entering the scanner room: You will lie on the scanning table (also called the gantry table or bore table). The technologist will position you correctly — typically on your back, arms above your head for abdominal scans.
- The scan: The table will move smoothly into the gantry. You will hear buzzing, clicking, or whirring sounds — these are normal and are caused by the rotating X-ray tube. The technologist observes you through a window and communicates via an intercom.
- Breath-hold instructions: For chest CT, you will be asked to take a deep breath and hold it for 5-15 seconds. This reduces motion blur and improves image quality. The machine will give audio instructions.
- Contrast injection (if applicable): The power injector will deliver the contrast. You may feel a warm flush spreading through your body, a metallic taste in your mouth, and a sensation as though you have urinated (you have not). These sensations are normal and pass in 30-60 seconds.
- End of scan: The table slides out. The technologist removes your IV catheter. You can usually resume normal activities immediately.
How Long Does a CT Scan Take?
- The actual scan: 5-15 seconds to 5-10 minutes, depending on the body part and whether contrast timing is needed.
- Total appointment time: 30-60 minutes, including preparation, IV placement, waiting (for oral contrast or reaction observation), and discharge.
- CT colonography: Approximately 2-3 hours total including bowel preparation and scan.
Is a CT Scan Painful?
The CT scan itself is entirely painless — you feel nothing from the X-rays. Sources of minor discomfort may include: the IV catheter insertion, lying still on a firm table (particularly uncomfortable for patients with back pain), and the brief warm/metallic sensation from IV contrast injection. If you have severe back pain, inform the technologist so they can use positioning aids.
Managing Claustrophobia
CT scanners are wide, open, ring-shaped doughnuts — far less enclosed than an MRI machine. Most patients do not experience significant claustrophobia in CT. However, if you are anxious, options include: verbal reassurance from the technologist via the intercom, a mild oral benzodiazepine (e.g., lorazepam) prescribed before the scan, and being accompanied by a support person to the scanner room (they will step out during the scan itself).
Image Quality Issues & Common Artifacts
An artifact in medical imaging is any feature in an image that does not correspond to actual anatomy. Artifacts can obscure pathology or mimic disease. Understanding them helps patients appreciate why some scans need to be repeated or why certain findings need further evaluation.
Streak Artifacts (Metal Artifacts)
Cause: Dense metallic objects (hip prostheses, dental fillings, spine instrumentation, bullet fragments) block X-rays almost completely, creating characteristic bright and dark streaks radiating from the metal. This is the most commonly encountered artifact in clinical CT. Metal Artifact Reduction (MAR) algorithms are now available on modern scanners to partially correct this.
Beam Hardening
Cause: As a polychromatic X-ray beam passes through dense tissue, lower-energy photons are preferentially absorbed, leaving only higher-energy (‘harder’) photons. This causes the center of dense structures to appear falsely dark. Classic example: a dark streak between the petrous bones of the skull base on brain CT — this does not represent actual pathology.
Motion Artifacts
Cause: Patient movement during the scan (breathing, heartbeat, bowel peristalsis) causes blurring or ghosting. Breath-hold instructions minimize respiratory motion for chest CT. Cardiac gating (synchronizing acquisition to the ECG) is used for coronary CT to freeze heart motion.
Partial Volume Effect
Cause: When a small structure straddles the boundary between two CT slices, the image averages the two, causing the structure to appear blurred or falsely merged with adjacent tissue. Thinner slice thickness reduces this artifact.
Ring Artifacts
Cause: Malfunction of one or more detector elements creates concentric rings on the image. This is an equipment-related artifact requiring service and calibration of the scanner.
Interpreting Your CT Results
Who Reads Your CT Scan?
CT images are interpreted by a radiologist — a physician who has completed medical school plus a minimum of 5 years of postgraduate radiology training (including a fellowship). Some radiologists sub-specialize further in neuroradiology, cardiothoracic radiology, or musculoskeletal radiology. The radiologist reviews your images on a DICOM workstation, adjusting ‘window’ and ‘level’ settings to optimize visualization of different tissues (bone window, soft tissue window, lung window).
Understanding Your Radiology Report
Your CT report consists of several standard sections:
- Clinical indication: Why the scan was ordered (e.g., ‘abdominal pain, query appendicitis’).
- Technique: What type of CT was performed (e.g., ‘CT abdomen/pelvis with IV and oral contrast, helical acquisition’).
- Findings: A systematic description of everything the radiologist observed, organ by organ. This section may contain technical language.
- Impression (or Conclusion): The most important section — the radiologist’s summary and diagnosis. Your referring doctor primarily uses this section. Read this first.
- Recommendations: Suggestions for further imaging, clinical correlation, or follow-up (e.g., ‘follow-up CT in 3 months to assess stability of 6mm lung nodule’).
Common Report Terms Explained
- Hyperdense: Appears brighter than surrounding tissue on CT — typically blood, calcium, or dense contrast.
- Hypodense: Appears darker than surrounding tissue — typically fluid, fat, or edema.
- Isodense: Same density as surrounding tissue — can make lesions hard to see without contrast.
- Enhancing: A lesion that becomes brighter after contrast injection, suggesting active vascularity (common in tumors and infections).
- Incidentaloma: An incidental finding discovered on a scan performed for an unrelated reason. Most are benign (e.g., small adrenal adenoma, liver cyst), but may require follow-up imaging to confirm stability.
- Indeterminate: The CT cannot definitively characterize a finding. Further imaging (often MRI or PET-CT) or biopsy may be recommended.
- No acute abnormality: No urgent pathology found. Does not necessarily mean everything is completely normal — subtle chronic changes may not be detailed in this summary.
How to Access Your CT Images
You have a legal right to your medical imaging. Options to obtain your CT images include:
- Patient portal: Many hospital systems now provide access to radiology reports and sometimes images directly through an online patient portal (e.g., MyChart, Patient Access).
- CD/DVD or USB drive: Request a copy from the radiology department. Images are stored in DICOM (Digital Imaging and Communications in Medicine) format, a universal standard readable by free DICOM viewers such as RadiAnt or Horos.
- Your referring doctor: Your doctor will receive the report automatically and can walk you through the findings at your follow-up appointment.
Cost, Insurance & Access
Cost is a major concern for patients, yet it is rarely discussed on clinical radiology websites. Here is what you need to know:
How Much Does a CT Scan Cost?
- United States: Without insurance, CT scan costs range from approximately $300 (simple head CT at an imaging center) to $6,000+ (complex multi-phase cardiac CT at a hospital). The average cost for an abdominal CT is approximately $1,200-$3,000. Costs vary significantly between hospital outpatient departments and independent imaging centers — the latter are typically 40-70% cheaper.
- United Kingdom (NHS): CT scans are free at the point of care for patients with a valid clinical referral.
- Australia (Medicare): Bulk-billed or partially subsidized for referred scans.
- Global average: $100-$500 USD in many middle-income countries.
Insurance Coverage & Prior Authorization
- Medical necessity: Most insurance plans (including Medicare and Medicaid in the US) cover CT scans that are medically necessary. Coverage for CT screening programs (e.g., lung cancer screening) may require meeting specific eligibility criteria.
- Prior authorization: Many insurers require your doctor to obtain pre-approval before a CT scan is performed. Failure to obtain prior authorization may result in denial of coverage or a significantly higher out-of-pocket cost.
- Deductibles and copays: Even with insurance, you may owe your deductible (up to $1,000-$7,000+) or a copay/coinsurance. Contact your insurer in advance to understand your out-of-pocket liability.
- Price transparency: In the US, hospitals are now legally required to publish their standard charges. Use this to compare prices before scheduling.
FAQ
Is a CT scan safe?
Yes, CT scans are considered safe for most adults when clinically indicated. They use low-dose ionizing radiation. The diagnostic benefit — catching a life-threatening condition such as stroke, pulmonary embolism, or cancer — almost always outweighs the small theoretical long-term cancer risk. Your radiology team applies the ALARA principle to minimize your dose.
How long does a CT scan take?
The actual scan takes between 5 seconds and 10 minutes, depending on the body part. Your total appointment — including check-in, IV placement, oral contrast waiting time, and post-scan observation — typically runs 30-60 minutes.
Can I eat before a CT scan?
It depends on the type of scan. If you are receiving IV contrast, fast (no solid food) for 3-4 hours beforehand. You can usually drink clear liquids. For non-contrast CT scans, no fasting is needed. CT colonography requires a full bowel prep the night before. Always follow your radiology department’s specific instructions.
Does a CT scan show cancer?
Yes, CT is a primary tool for cancer detection, staging, and monitoring. It can identify tumors, assess their size and local invasion, detect lymph node involvement, and identify distant metastases. However, very small lesions may not be visible, and some CT findings cannot definitively distinguish between benign and malignant tissue — which is why additional tests (PET-CT, MRI, biopsy) are sometimes needed.
What is the difference between a CT scan and a CAT scan?
There is no difference — they are the same procedure. ‘CAT scan’ (Computerized Axial Tomography) is the original term coined in the 1970s. ‘CT scan’ (Computed Tomography) is the modern, universally preferred terminology.
Will my insurance cover a CT scan?
Most health insurance plans cover medically necessary CT scans, but you may owe your deductible, copay, or coinsurance (typically $50-$500 per scan with insurance). Many plans require prior authorization. Contact your insurer before scheduling to confirm coverage and estimate your out-of-pocket cost.
What should I do if I am claustrophobic?
Tell your doctor and the radiology team in advance. CT scanners are wide, open rings — much less enclosed than MRI machines. Most claustrophobic patients tolerate CT without difficulty. If you remain anxious, your doctor can prescribe a mild oral sedative (e.g., lorazepam) to take before the scan. You should arrange transport home if taking sedation.
How do I get the images from my CT scan?
You can request a copy of your CT images from the radiology department on a CD, DVD, or USB drive. They are stored in DICOM format, which can be viewed using free software (RadiAnt Viewer, Horos on Mac). Many hospitals also offer images through an online patient portal. You have a legal right to your own medical records.
Conclusion
Computed Tomography remains one of the most transformative and versatile tools in modern medicine. From a 30-second trauma scan in the emergency room to a millimeter-precise lung cancer screening study, CT offers an unmatched combination of speed, detail, and accessibility.
Understanding how CT works, when it is used, what the real risks are, and how to prepare and interpret your results empowers you to be an active participant in your own healthcare. The key takeaways from this guide are:
- CT uses ionizing radiation to create detailed cross-sectional images — the diagnostic benefit almost always outweighs the small radiation risk.
- Modern CT scanners are fast, and the procedure is painless. Most scans take 5-10 minutes.
- Contrast media greatly enhances imaging but requires disclosure of kidney function, diabetes, allergies, and pregnancy.
- Your radiologist’s Impression section is the most important part of your report.
- Emerging technologies — photon-counting CT and AI reconstruction — promise higher image quality at lower doses, driving CT into an exciting future.
Always consult your physician or radiologist for guidance specific to your clinical situation. This guide is intended for educational purposes and does not substitute for individualized medical advice.
Adrian Cole is a technology researcher and AI content specialist with more than seven years of experience studying automation, machine learning models, and digital innovation. He has worked with multiple tech startups as a consultant, helping them adopt smarter tools and build data-driven systems. Adrian writes simple, clear, and practical explanations of complex tech topics so readers can easily understand the future of AI.